The experience of depression manifests in two different forms, making it crucial to understand the difference between major depressive disorder and persistent depressive disorder. Both disorders fall within the realm of depression but differ in their intensity and severity as well as the impact it has on your health.
The major depressive disorder is identified by its short-term and intense effect. Persistent depressive disorder as the name suggests is persistent and long-lasting. Both these disorders have a severe negative influence on the health of an individual. According to research by the World Health Organization, depression is the second-leading cause of disability in the world and is projected to rank first by 2030 associated with high rates of suicidal behavior and mortality. Therefore, it’s necessary to bring this problem into focus and address it before it starts interfering with your work and personal life.
In this blog, we’ll discuss the key difference between major depressive disorder and persistent depressive disorder. We’ll also dive deeper to uncover some helpful strategies and tools to help you manage your disorder effectively. Read on to learn more!
Depression is tough, but recovery is possible!
Whether it’s medication, therapy, or healthy habits—solutions are out there. Don’t let depression hold you back from the life you deserve.
Lighten the Load Today
866.939.6292
Understanding the difference between major depressive disorder and persistent depressive disorder
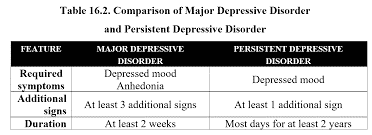

Both major and persistent depressive disorders are chronic conditions that create an environment of stress and worry. This stress is not your normal stress that withers away easily but one that degrades peace of mind and interferes with work and relationships. The main difference between major depressive disorder and persistent depressive disorder lies in its intensity, severity, and duration of occurrence. While major depressive disorder has an intense negative impact on the mind, it usually lasts for a short term like for a week or so. When it comes to persistent disorder, it is usually less empowering but long-lasting.
For example, let’s consider a situation where a student gets a bad grade on an exam. For a few weeks, the student is depressed because of the sadness of the score. After some time, the sadness subsides and the student is happy again. This behavior can be labeled as major depressive disorder. However, with the persistent disorder, the sadness persists and the student is not happy or excited about anything even after recovering from the sad state.
What is Major Depressive Disorder (MDD)?
Major Depressive Disorder (MDD) is a mental health condition where a person feels very sad, hopeless, or loses interest in activities for at least two weeks. It affects daily life, making it hard to work, study, or enjoy life. Symptoms include changes in sleep, appetite, energy levels, and concentration.
What is Persistent Depressive Disorder (PDD)?
Persistent Depressive Disorder (PDD), also known as dysthymia, is a long-term form of depression. People with PDD feel sad or down most days for at least two years. It affects daily life and can make it hard to enjoy things or stay motivated. Symptoms include low energy, trouble sleeping, and poor concentration.
Overlapping Symptoms of persistent and major depressive disorder
Symptoms of major and persistent depression can be identified through the following behavioral changes –
- Disinterest and lack of pleasure in everyday activities
- Persistent feelings of sadness and hopelessness
- Irregular sleep schedules and trouble sleeping
- Getting fatigued easily and being low on energy
- Having difficulty maintaining focus or clarity
- Experiencing self-criticizing thoughts and negative emotions
- Greater frequency of suicidal thoughts and attempts
- Increased restlessness or sluggishness
- Onset of persistent and depressive mood nearly every day
- Difficulty in thinking or making decisions
- Significant impairment in social, occupational, and other areas of life
What causes major and persistent depressive disorder?
Various biological, psychological, and social factors are responsible for the development of persistent and major depressive disorder in an individual. Let’s understand each of these causes in detail.
Biological Causes
- An imbalance in neurotransmitters such as serotonin, norepinephrine, and dopamine plays a major role in triggering depression in an individual, serotonin plays a more prominent role in the development of persistent depressive disorder.
- The genetic history of major depressive disorder is most likely to bring Major depressive symptoms in a person. While genetics also play a role in Persistent Depressive Disorder (PDD), the extent of genetic influence may be less pronounced compared to major depression.
- Certain chronic illness conditions such as diabetes, chronic pain, and thyroid disorders can be responsible for the occurrence of major depression. Medical conditions are less likely to establish persistent depression, but chronic issues can still add stress and reduce well-being.
Psychological Causes
- Negative thinking and self-criticizing thoughts trigger depressive symptoms.
- Traumatic life experiences like loss, abuse, or any other such incident can be responsible for depressive thoughts. However, in the case of persistent depression, it’s chronic low-grade stress, rather than major life changes, which is responsible for the symptoms.
- Major depression is triggered by life events, while persistent depression is triggered by long-term stressors, unresolved interpersonal conflicts, and childhood adversity.
Social Factors
- Lack of social support during an emotional crisis.
- Chronic stress and challenges concerning a person’s economic condition.
- Childhood trauma and adverse life events, with early experiences and financial challenges, have a profound role in the development of persistent disorders.
Treatment and Diagnosis Approaches
Research says that for a doctor to diagnose major depressive disorder, a person must have experienced at least two of the depression episodes separated by at least 2 months
While for persistent depressive disorder, research suggests that, the symptoms cannot have been absent for more than 2 months at a time during 2 years, in adults, or 12 months, in younger people.
Treatment options
For Major Depressive Disorder
According to the National Center for Biotechnology Information (NCBI), depression-centered psychotherapy is generally considered an initial treatment for mild to moderate major depression. Based on substantial clinical evidence, two distinct psychotherapeutic approaches are recommended for its treatment: cognitive-behavioral (CBT) therapy and interpersonal (IPT) therapy.
For Persistent Depressive Disorder
The various treatment techniques suggested under this aim to manage long-term symptoms and improve overall functioning. A report by NCBI shows persistent depressive disorder responds well to several acute interventions, such as combined psychological and pharmacological treatments
The treatment options suitable for each of these disorders depend on person to person, on their circumstances and medical condition. More severe cases might require a combination of medication and therapy, while milder cases might benefit more from initial therapy with medication. It’s better to seek professional help who understands the difference between major depressive disorder and persistent depressive disorder well.
Your Journey to a Brighter Tomorrow
At Calusa Recovery, we empower you to overcome addiction and mental health challenges with personalized treatments that help you reclaim a healthier, fulfilling life
Help Me Transform My Life
FAQs
Que: Can people with persistent depressive disorder feel happy?
Ans: Yes, people with persistent depressive disorder can feel happy, but the feeling doesn’t last longer. Because of the persistent depressive disorder, the good feelings often get lost in the realm of negativity and compel the person to feel depressed.
Que: Can major depression be persistent?
Ans: There is a huge difference between major depressive disorder and persistent depressive disorder. Major depression typically lasts for two weeks or less, but it can be still persistent in some cases, depending on the nature of the depression and its symptoms. Some of these conditions include: having another episode of major depressive disorder while recovering from a previous episode, experiencing multiple episodes within one year, or being resistant to treatment for major depressive disorder
Que: Can you have MDD and PDD?
Ans: Yes, one can have MDD and PDD together. The co-occurrence of both depressive disorders is termed double depression. Double depression is characterized by low persistent depressive disorder and a more intense MDD. However one needs to understand the difference between major depressive disorder and persistent depressive disorder to spot their co-occurrence easily
Que: Is persistent disorder worse than MDD?
Ans: Both persistent disorder and MDD have a different impact on health. The effects of the persistent disorder are less severe and long-lasting. MDD, on the other hand, is more severe and short-term. It brings an immediate impact on work, relationships, and health unlike persistent which brings a pervasive impact
Que: What are the symptoms of persistent depressive disorder?
Ans: A core feeling of sadness and emptiness in life characterizes Persistent Depressive Disorder. It is accompanied by other symptoms such as appetite change, sleep disturbances, fatigue, and lack of focus.
Conclusion
Coping with depressive disorder becomes difficult when the symptoms are neglected. As you gain a better understanding of the symptoms and treatment options, it will be easier for you to make the right decision to recover. Recovery will come with its own set of challenges, but with awareness and confidence, you’ll be able to manage it well. Now that you understand the difference between major depressive disorder and persistent depressive disorder, you’ll be better equipped to seek the right treatment. Let loose of all the negativity and fear of judgment. Your path to a healthier you will begin with it! Get in touch with Calusa Recovery for the best treatment for Major Depressive Disorder and Persistent Depressive Disorder.