Major depressive disorder (MDD), also referred to as major depressive disorder, is a scientific term that encompasses a wide range of emotions. It is not simply a state of sadness or a period of difficulty. It is a medical condition that necessitates comprehension, treatment, and a great deal of support from the family. Let us explore the following topics: Major depressive disorders and major depressive disorders symptoms.
What are Major Depressive Disorders and their Symptoms?
Major Depressive Disorders, also known as clinical depression is one of the most serious mood disorders that affects you as well as the people around you. Various depressive disorders symptoms that affect how you feel, think, and handle daily activities including sleeping, eating, or working.
The depressive disorders symptoms must be present for at least two weeks so that it can be diagnosed as a disorder. This mental health condition is debilitating and will lead to a variety of emotional and physical problems.
The Significance of Grasping Major Depressive Disorder
It’s really important for everyone, not just those going through it, to grasp what Major Depressive Disorder is all about. When we get a handle on it, it means we can spot it early, find the right treatment, and handle it better. Plus, when we understand this disorder, we can start chipping away at the stigma around mental health. That way, more folks will feel comfortable reaching out for support when they need it.
Let’s chat about how common it is and how it affects people and society.
You know, Major Depressive Disorder is pretty common in the United States. According to the National Institute of Mental Health, about 7% of adults here have gone through at least one major depressive episode in the past year. That’s like 17.3 million folks dealing with it.
MDD doesn’t just hit individuals; it also has a big ripple effect on society too. According to the World Health Organization (WHO), depression is the top cause of disability across the globe. It can mess with how people perform at their jobs, put a strain on their relationships, and in really serious cases, it can even lead to suicide. So, the price society pays because of depression is huge, and that’s why it’s such a major public health concern.
Exploring Major Depressive Disorder isn’t just something for textbooks; it’s vital in our mission to boost mental health and happiness together. As we dig deeper into the details of this condition in the next parts, keep in mind that knowing about it gives us an upper hand. The more we get how it works, the better we can tackle it, be there for those going through it, and, in the end, shrink its effects on our community.
Let’s talk about what we mean when we say ‘Major Depressive Disorders.
You know, when we talk about Major Depressive Disorder (MDD), it’s basically what we usually call depression. It’s a pretty serious mental health condition where you’re stuck feeling really sad, and hopeless, and you lose interest or joy in the things you normally enjoy. The tricky thing about MDD is that these feelings aren’t just a passing phase; they stick around for at least two weeks or even longer. It’s not just a case of having a bad day or feeling down after a tough time – this is a complex issue that can affect anyone, no matter their age.
Understanding Recurrence in Major Depressive Disorder (MDD)
In the world of MDD (that’s Major Depressive Disorder, by the way), when we say “recurrent,” we’re basically talking about folks who’ve dealt with more than one bout of major depression. So, picture this: someone goes through their first round of major depression and then decides to make a comeback a few times in their life. These comebacks can be sparked by specific life events, or they can just pop up out of nowhere. The important thing to remember here is that even if someone has only faced that big D (major depressive episode) once, they’re still in the MDD club. It’s all about the symptoms and how heavy they hit, not how often they show up.
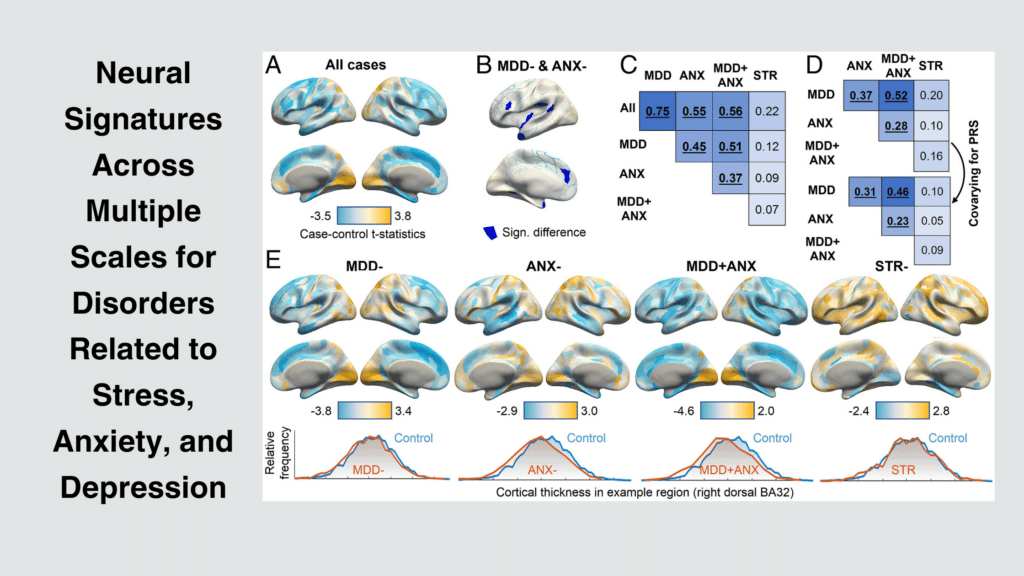
When we talk about how serious a case of MDD is, we use the term “moderate” to describe how intense the symptoms are. You see, major depressive episodes can be divided into three categories: mild, moderate, and severe. A moderate episode falls in the middle, meaning the symptoms are pretty tough and can really get in the way of your daily life, but it might not be as all-consuming as a severe episode. But here’s the important thing to remember: just because it’s called “moderate” doesn’t mean it’s not a big deal. Even a moderate episode of MDD needs attention and treatment.
Feelings of Major Depressive Disorder.
Basically, when we talk about Major Depressive Disorder, we’re looking at recognizing those ongoing, all-encompassing feelings of sadness and hopelessness that really mess with your everyday life. Terms like “keeps coming back” and “not too extreme” help doctors figure out how often and how bad these feelings are, which helps them decide on the best way to treat them So, just keep in mind that getting a handle on these definitions is the first thing to do if you want to spot and deal with this pretty common mental health problem.
How to Recognize the Symptoms of Major Depressive Disorders?
To really get a grip on any condition, especially one as tricky as major depressive disorder (MDD), you’ve got to start by getting cozy with major depressive disorder symptoms. Think of these as the little flags that say, “Hey, something might be up,” and they’re pretty darn important in nudging someone toward seeking some assistance. But, here’s the kicker: MDD symptoms are like a mixed bag of surprises. They’re different for everyone, both in terms of what’s showing up and how intense they can get.
What are the common symptoms of Major Depressive Disorders?
When someone’s dealing with MDD, they often go through a bunch of symptoms that stick around for at least two weeks. These typical signs of major depressive disorder include things like feeling really sad, empty, or like there’s no hope in sight, and these feelings just won’t let up. Plus, you might lose interest in stuff you once loved, notice changes in your appetite or weight, struggle with sleep (either too much or too little), and constantly feel tired or low on energy.
And it’s not just physical stuff – your mind can get in on the action too. You might find it hard to think straight, concentrate, or make decisions. Sometimes, those thoughts of death or suicide can pop up too. But hey, don’t ever think these symptoms mean you’re weak or have a bad character. They’re just part of the illness, and the good news is, they can be treated effectively. So, remember, there’s hope and help out there!
What are the variations in Depressive disorder symptoms and their impact on Daily Life?
When it comes to Major Depressive Disorder (MDD), it’s important to know that the way it shows up can vary a lot from person to person.
For some folks, depression can show itself through physical stuff like never-ending headaches, tummy troubles, or ongoing aches and pains.
Meanwhile, others might feel it more emotionally, dealing with things like a heap of guilt, feeling like they’re not worth much, or having that constant feeling of anxiety. It’s a real mixed bag!
The impact of these depressive disorders symptoms in your daily life can be pretty hefty. They can seriously mess with your productivity, put some strain on your relationships, and make even the simplest tasks feel like a big challenge. What’s worse, these effects can snowball – the symptoms lead to some not-so-great life experiences, which, in turn, can make the symptoms even worse.
Now, recognizing these symptoms is super important, and not just because you want to put a name on it. Knowing exactly how MDD is affecting you can help figure out the best ways to deal with it. This can mean lessening the intensity of those symptoms, improving your overall quality of life, and getting a better handle on this condition.
But remember, if you or someone you know is showing these signs, it doesn’t automatically mean it’s MDD. These depressive disorders symptoms could be tied to other stuff going on in your life, or maybe just some tough situations you’re facing. However, if these symptoms don’t let up, it’s really crucial to reach out to a mental health pro. They can give you a proper diagnosis and steer you toward the right treatment options.
ICD-10 Classification for Major Depressive Disorders.
Before we jump into the nitty-gritty details of how we classify major depressive disorders, let’s first get to know the tool we use for diagnosis – the ICD-10. The International Classification of Diseases, 10th Revision (ICD-10), is like the global dictionary for categorizing all sorts of illnesses, including mental health issues. It’s the brainchild of the World Health Organization (WHO), and it’s pretty much the gold standard worldwide.
Now, why is this ICD-10 so important, you ask? Well, it’s like the secret sauce behind diagnosing conditions like major depressive disorders. It gives healthcare pros a common language to talk about health stuff, no matter where they are in the world. Plus, it’s a powerhouse for research and getting a deeper understanding of these conditions. With ICD-10, we keep things consistent when diagnosing and treating medical conditions, making sure everyone’s on the same page, no matter where they practice.
How does ICD-10 classify the Major Depressive Disorders?
In the ICD-10, they put major depressive disorders in the mood disorder section. They use the code F32 for one-time episodes and F33 for when it keeps happening. But remember, these codes don’t just sort things; they also tell you how bad it is and some details about the disorder.
So, when we’re talking about F32 and F33 classifications, they come with a little number tag to show how serious things are. For example, ‘F32.0’ means you’re dealing with a mild case of feeling down, and ‘F32.2’ means it’s a more severe version without any of those weird psychotic symptoms. Now, if we switch to the ‘F33’ category, it pretty much works the same way but for when you’re having those recurrent depressive episodes.
This way of organizing major depressive disorders helps doctors diagnose them more accurately, so they can create treatment plans that work better. When doctors think about things like how many times someone has felt this way, how bad it’s been, and whether they’ve had any strange thoughts, it helps them give the right treatment to each patient.
Basically, ICD-10 does more than just sort things out. It really helps us grasp how serious and complicated major depressive disorders are, which is a big deal in our efforts to handle and eventually beat this tough condition.
What are the treatment options for Major Depressive Disorders?
One really important thing when dealing with major depressive disorder is knowing about the different ways to treat it. Just like how the symptoms can be different for each person, the treatments that work best can also vary. The main aim is to make the depressive disorder symptoms less severe, make life better, and help with recovery.
Medication
Using medication is a pretty common way to treat major depressive disorders, and a lot of times, doctors like to start with antidepressants. You might have heard of ones like Prozac or Zoloft, which are called selective serotonin reuptake inhibitors (SSRIs), or there are also serotonin and norepinephrine reuptake inhibitors (SNRIs). Basically, these meds help change the balance of certain chemicals in your brain that affect your mood. But just so you know, how well a medication works can be different for each person, and it might take a bit of trying to find the right one for you. All medications can have some side effects, so it’s important to talk to your healthcare provider about that.
Therapy
When it comes to dealing with major depressive disorders, there are a couple of ways to go about it. One way is through something called psychotherapy, or you might have heard it being called “talk therapy.”
One type of talk therapy is called Cognitive-behavioral therapy, or CBT for short. This one’s all about helping you spot and fix those negative thoughts that make you feel down.
Then there’s interpersonal therapy or IPT. This one’s more about making your personal relationships better, which can really help with your depression. And don’t forget about group therapy. It’s where you get together with a bunch of folks who are going through similar stuff. You chat, share stories, and learn how to cope better. It’s like a support group, and it can really help.
Changes in Lifestyle
Dealing with major depressive disorders usually involves meds and therapy, but your lifestyle can also be a big player in managing them. Stuff like getting regular exercise, eating balanced meals, getting enough sleep, and cutting back on booze can really help your mental health. And don’t forget about mindfulness tricks like meditation, taking deep breaths, or trying out yoga – they’re great for handling stress and keeping a positive mindset.
The Importance of Personalized Treatment Plans
Because major depressive disorders are pretty complicated, it’s super important to have a personalized treatment plan. See, everyone’s experience with depression is unique, so trying to use the same treatment for everyone doesn’t really cut it. Instead, a personalized plan looks at things like how bad the symptoms are, what kind of symptoms you have, your health history, if you’ve got any other mental or physical issues, and your own preferences and lifestyle. And here’s the thing, it’s an ongoing thing that means you’ll need to check in with your healthcare peeps regularly to see how you’re doing and maybe change things up if needed.
Dealing with major depressive disorder might feel tough, but it’s essential to know that there are plenty of ways to tackle it. Working closely with your healthcare team to craft a treatment plan that’s just right for you can truly change the game. Having major depressive disorder doesn’t mean you should settle for just getting through life; it’s about thriving and living your best life.
Spravato Treatment
The medicine called esketamine is known as Spravato when used along with a pill for treating major depressive disorder (MDD) in grown-ups. It’s meant for adults who didn’t get better with other medicines, a condition known as treatment-resistant depression.
Spravato is a nasal spray given by a doctor because it can have serious side effects and may be misused. It works by affecting a different brain chemical called glutamate, which is unlike most regular antidepressants. This offers a new way to treat depression. As of September 2021, doctors thought Spravato treatment was a promising but relatively new option. If you wanted the most up-to-date information, you should have talked to your doctor.
What is Spravato Nasal Spray?
The FDA gave the green light to Spravato nasal spray, also known as esketamine nasal spray, for treating depression. Some people think it’s a huge step forward in mental health over the last 50 years.
Spravato treatment works by focusing on certain parts of the brain called NMDA receptors, which are thought to be involved in depression. By adjusting these receptors, Spravato helps bring back balance to the brain’s chemicals, which makes people feel better and happier. You can use it on its own or with regular antidepressant pills.
Spravato has a big advantage – it works quickly. Unlike regular antidepressants that can take weeks or even months to help, studies show that Spravato can quickly help people with tough-to-treat depression.
But there are some important things to know. Spravato can make you feel sleepy or disconnected, so doctors need to watch you closely after you take it. Also, some people might misuse Spravato, so doctors should give it to you with care. And remember to tell your doctor if your mood or actions change, because Spravato might increase the chances of having bad thoughts or actions.
Spravato’s Dosage for Depression Treatment
A doctor decides how much Spravato to give based on the patient’s health, how they’re doing with the treatment and other things. The doctor usually gives the medicine through the nose in a special place, while watching over it. At first, they often give it two times a week for the first month, then once a week for the second month. Depending on how the patient is doing, they might give it less often, like once every two weeks, or they might keep giving it every week. Remember, always take Spravato with a pill for depression. Like any medicine, it’s very important to follow what the doctor says to make sure it works well.
Form and Strength
Spravato, also known as esketamine, comes in two nasal spray strengths: 28 mg and 56 mg. The right strength and dose for your treatment will be decided by your healthcare provider. It is based on factors like your medical condition and how you respond to the treatment. Always remember, that you should only use Spravato under the guidance of a healthcare professional. Because it can have side effects and a risk of misuse or abuse.
Dosages
A doctor decides how much Spravato (esketamine) nasal spray you need based on your health. Like how you’re doing with the treatment and other things. They give you the spray in a special healthcare place, and someone watches over you.
At first, the doctor usually tells you to use it two times every week for a month. Then, in the next month, you only need it once a week. After that, it depends on how you’re feeling. They might tell you to use it once every two weeks or keep using it every week.
It’s super important to do exactly what the doctor says to make sure it works the best. If you want to know more that’s just for you, talk to your doctor.
Dosage for people with Suicidal Thoughts or Behaviors
When dealing with Major Depressive Disorder (MDD) and thoughts of self-harm. The doctors might think about adding Spravato to the treatment plan. Remember, it’s the healthcare pros who should figure out how much to give, taking into account the patient’s history. How bad the symptoms are, and how well other treatments worked before. Usually, they give Spravato in a healthcare place where they watch over you.
At first, you might get Spravato twice a week for a month. After seeing how it works for you, they might reduce it to once a week or maybe less often. Like once every two weeks, from the third month on. Keep in mind, though, that Spravato is just one piece of the puzzle. It works best when you also take an oral antidepressant, talk to a therapist, and make some lifestyle changes. And with any medicine, they’ll keep a close eye on how you’re doing and if there are any side effects.
We at Calusa Recovery, provide Spravato Treatment for people with depression. We are a certified Spravato Treatment Center in Fort Myers, Florida.
Conclusion
In this thorough guide, we’ve gone deep into Major Depressive Disorder (MDD). We’ve talked about what it is, how to recognize its signs, the Spravato Treatment, and its ICD-10 category. We’ve also looked at ways to treat it and given some advice on living with MDD.
But it’s essential to understand that your journey in dealing with MDD doesn’t stop here. We’ve stressed that even if you have MDD, you can still lead a fulfilling life. The right treatment, support from others, and taking care of yourself can help with symptoms and make your life better. Always remember that MDD doesn’t define you or limit your potential for happiness and success.
Professional help is necessary
While this guide has a lot of information, know that it can’t replace advice from a medical pro. If you or someone you know is showing signs of MDD, get in touch with a mental health expert. They can give you a proper diagnosis and make a plan that’s just right for you.
It might feel scary to reach out, but it’s a big step toward getting better. Remember, asking for help doesn’t mean you’re weak. It shows strength and self-awareness. You’re not alone in this, and there are resources like Relevance Recovery to guide you through tough times.
Let’s stop making mental health issues seem shameful. We should talk about them, understand them, and, most importantly, get help when we need it. Mental health is important, and so are you!