1 out of 4 teenagers say they have at least once abused or misused prescription medication. When something you once found enjoyable becomes indispensable, you are said to be suffering from addiction. According to medical professionals, drug addiction is characterized by an insatiable need for a drug, compulsive and out-of-control drug use, and persistent drug use in spite of negative outcomes. Because they stimulate strong reward centers in the brain, opioids are extremely addictive. The difficult journey of opioid withdrawal timeline occurs in the shadow of the opioid epidemic, where innumerable lives are lost to addiction. This battle is silent but crucial. Numerous communities have been affected by the opioid crisis, which has wreaked havoc in its wake. We take a deep dive into this crisis in this blog, concentrating on the terrifying phase of withdrawal. It’s a story that calls for empathy, understanding, and a concerted effort to escape the bonds of dependency.
Opioid and its forms
Prescription drugs and illicit substances fall under the category of opioids. They are well known for their capacity to interact with the brain’s and other body’s opioid receptors, resulting in the alleviation of pain and a euphoric feeling. Although they are frequently prescribed to treat moderate to severe pain, opioids carry a significant risk of addiction and abuse.
Opioids come in a number of forms, such as:
- Prescription Opioids: Medical practitioners usually recommend these to treat pain. Among the frequently prescribed opioids are morphine, fentanyl, hydrocodone, and oxycodone
- Heroin: Made illegally from morphine, heroin is an opioid with a high potential for addiction.
- Synthetic Opioids: Some opioids are made entirely of synthetic materials. One strong synthetic opioid used medicinally for extreme pain is fentanyl, but because of its potency, there is a significant risk of overdosing
What is Opioid addiction?
Opioid addiction sometimes referred to as opioid use disorder (OUD), is a long-term medical condition marked by obsessive and problematic opioid use. Opioids are a class of drugs that includes heroin, an illegal drug, and synthetic opioids like fentanyl and hydrocodone, which are prescribed painkillers.
Opioid receptors are specialized receptors found in the brain and spinal cord that opioids bind to in order to function. These receptors have the ability to block pain signals and cause relaxation and pleasure when they are activated. Opioid abuse or prolonged use, however, can result in tolerance, dependence, and addiction.
Addiction to opioids is a multifaceted illness that involves both psychological and physical aspects. Massive consumption of opioids makes a person physically dependent on others for their needs. It has the potential to impact individuals from diverse backgrounds, and its origins could be impacted by behavioral, environmental, and genetic factors.
The overprescription of opioid painkillers has contributed to the opioid epidemic, which has made it more urgent than ever to address opioid addiction as a public health emergency. Moving forward, we will be discussing the opioid withdrawal symptoms and timeline for you to understand and treat opioid addiction timely.
Opioid Addiction Symptoms
It can be difficult for people who are addicted to opioids to stop using these drugs, which can have negative effects on their relationships, general well-being, and health. The following are some of the main traits of opioid addiction:
- Loss of Control: Even when they are aware of the harmful effects of their opioid use, people who are addicted to these drugs frequently struggle to stop using them.
- Craving: An intense, enduring need or craving for opioids can push someone to use them even in the face of detrimental consequences to their life.
- Tolerance: People may grow tolerant to opioids over time, requiring higher dosages to produce the desired results.
- Physical Dependency: When opioids are used continuously, the body develops a dependence on them, and stopping use can cause withdrawal symptoms like aches in the muscles, sweating, nausea, and anxiety.
- Social and Occupational Impairment: Addiction to opioids frequently makes it difficult for a person to carry out their obligations at home, at work, or at school. Relationships may suffer, and social isolation may result.
- Continued Use Despite Harm: Because opioid addiction is compulsive, people with the disorder continue to use opioids despite suffering negative outcomes.
What opioid withdrawal is all about?
With increased consumption, our body becomes dependent on opioids and the body’s reaction to stopping opioid use suddenly or drastically reducing it is known as opioid withdrawal. These substances, whether purchased legally or obtained illegally, attach to opioid receptors in the brain to relieve pain and produce euphoria. Long-term use of these drugs, however, causes the body to become dependent on them, which can cause a range of negative emotional and physical effects when the use is stopped.
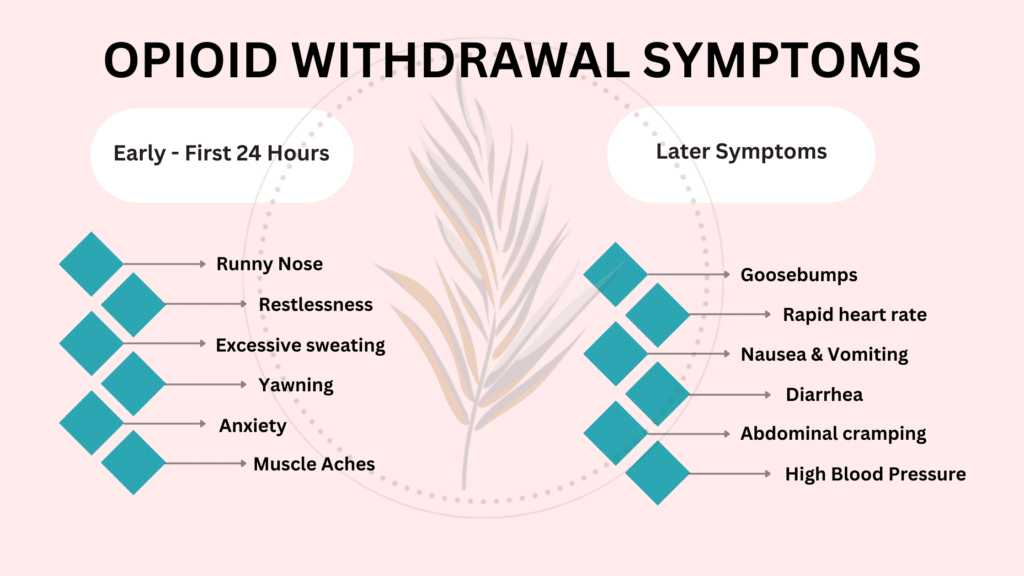
A variety of symptoms, from physically uncomfortable to emotionally taxing, frequently accompany the onset of opioid withdrawal. Muscle aches, nausea, vomiting, diarrhea, and insomnia are examples of physical symptoms. Those who want to escape the bonds of addiction may find it extremely difficult to overcome these severe and crippling manifestations. Withdrawal symptoms can vary greatly in severity and duration, depending on several factors including the kind of opioid used, how long it was used for, and individual metabolic differences.
Medications like methadone, buprenorphine, or naltrexone are examples of medical interventions for opioid withdrawal that can help control cravings and lessen some of the physical symptoms. These drugs are frequently used in conjunction with a more comprehensive approach called medication-assisted treatment (MAT), widely known as a medical detox program, well-known for its effectiveness in promoting healing.
Opioid withdrawal timeline
Opioid withdrawal typically occurs in phases, each distinguished by unique symptoms. During the first 24 hours following the last opioid use, there is an early phase that is marked by anxiety, restlessness, and a spike in flu-like symptoms. Physical symptoms worsen as withdrawal goes on and peak on the second or third day. Eventually, physical symptoms gradually go away in the later stages, but psychological symptoms like depression and cravings might last for a long time.
Depending on variables like the kind of opioid taken, how long it was used for, how much was taken, and individual differences in metabolism, the time required to taper off an opioid can differ greatly from person to person. Compared to long-acting opioids, withdrawal from short-acting opioids usually starts sooner after the last use. Here’s what an ideal opioid withdrawal timeline looks like-
Early Phase
- Within the first six to twelve hours following the last use, early withdrawal symptoms may appear.
- Anxiety, yawning, runny nose, restlessness, and increased tears are common early symptoms.
- People may have increased pain sensitivity, insomnia, and aches in their muscles.
Peak Affection
- The height of the withdrawal symptoms usually occurs in the first 24 to 72 hours following the last opioid use.
- The physical symptoms worsen and can include chills, sweating, nausea, vomiting, diarrhea, and cramping in the abdomen.
- There may be noticeable psychological symptoms like irritability and anxiety. People may get flu-like symptoms, which makes this stage especially difficult.
Subacute Withdrawal
- For the next 3-4 days, physical symptoms progressively start to lessen following the initial peak.
- Emotional symptoms like depression, mood swings, and difficulty concentrating can be evident, and cravings may continue.
- Sleep disturbances and low energy levels might persist.
Acute Symptom Relief
- While some psychological symptoms may linger, acute withdrawal symptoms usually go away within the first week.
- Physical symptoms go away, including headaches, sweating, and upset stomach.
- Your sleep habits might start to get better.
Post-Acute Withdrawal
- After the acute withdrawal phase, some people may have post-acute withdrawal symptoms (PAWS), which can linger for weeks or months.
- Anxiety, depression, mood swings, and sleep disturbances are some of the symptoms of PAWS.
- While cravings might linger, they frequently get weaker with time.
It is important to remember that the opioid withdrawal timeline varies from person to person. The course of withdrawal can also be influenced by variables like the existence of co-occurring mental health conditions, the degree of social support, and treatment participation. You must seek expert medical advice and assistance during this process to ensure a safer and more comfortable withdrawal. Drugs like buprenorphine or methadone may be prescribed to treat withdrawal symptoms and assist patients on their path to recovery.
Road to Recovery
Opioid addiction treatment is a difficult but attainable path that calls for a variety of interventions, such as ongoing medical care, psychological support, lifestyle modifications, and sustained dedication. Less than 10% of those in need of such treatment are getting it, even though there are efficient treatment interventions for opioid dependence that can lower the risk of overdose.
This is a recovery road map that highlights important actions to take:
- Acknowledgment and Acceptance: Self-reflection and acceptance of our shortcomings are important and that’s the first step to curing it. Recognize that the addiction exists and that a change is necessary. Understand that healing is a process that takes time and effort to complete.
- Seek Professional Assistance: Be open to seeking professional help and accelerating your detox treatment. For guidance on the best course of action and an accurate assessment of the addiction, speak with a healthcare provider or addiction specialist. To safely manage withdrawal symptoms, think about enrolling in a detoxification program under medical supervision.
- Medication-Assisted Treatment (MAT): Under the guidance of a healthcare professional, investigate medication-assisted treatment options, such as methadone, buprenorphine, or naltrexone. MAT can facilitate long-term recovery, lessen withdrawal symptoms, and help control cravings.
- Therapy and Counseling: To address the psychological aspects of addiction, attend individual and group therapy sessions. Effective methods for altering thoughts and behaviors include contingency management and cognitive-behavioral therapy (CBT).
- Support Groups: To meet people going through similar struggles, go to support groups like SMART Recovery or Narcotics Anonymous (NA). Peer support offers understanding, encouragement, and a sense of belonging.
- Lifestyle Modifications: Take up a healthy diet, get enough sleep, and engage in regular exercise. Create a schedule that supports both mental and physical health.
- Recognize Triggers and Create Coping Mechanisms: Determine the circumstances, feelings, or surroundings that set off the urge to take opioids. To deal with triggers without turning to drugs, learn coping mechanisms like mindfulness, stress reduction, or substitute activities.
- Social and Family Support: Involve friends and family in your recuperation. Encourage wholesome connections and look for assistance from family members who comprehend and support the process of healing.
- Ongoing Monitoring and Treatment: Understand that recovery is a continuous process and that treatment modifications may be necessary as time goes on. Attend therapy sessions, support groups, and check-ups with your doctor regularly to track your progress and address any new issues that may arise.
- Relapse Prevention: Create a plan to prevent relapses that includes coping mechanisms for high-risk circumstances. Rather than seeing setbacks as failures, learn from them and turn them into opportunities for personal development.
- Rebuilding Life and Purpose: To re-establish stability and a sense of purpose, seek education, employment, or vocational training. Take part in things that make you happy, fulfilled, and proud of yourself.
- Celebrate Milestones with the community: Whether they are days without alcohol, reaching treatment objectives, or individual accomplishments, recognize and honor milestones. To improve society and strengthen a feeling of community, think about taking up advocacy or community service.
- Ongoing Support: Even after reaching first goals, stay involved in the recovery community and look for ongoing assistance. Encouraging relationships with others and expert guidance can be crucial for sustaining sustained rehabilitation.
Recovering is a personal and distinct journey; there isn’t a one-size-fits-all strategy. A longer-lasting recovery and a happier, healthier life are possible with a treatment plan customized to each patient’s needs and adherence to the regimen.
Frequently Asked Questions (FAQs)
How long do opioid withdrawal last?
Although the length of opioid withdrawal varies, the acute phase usually peaks one to three days following the last dose. During the first week, the physical symptoms gradually go away, but the psychological ones might linger. Symptoms of post-acute withdrawal (PAWS) may persist for several weeks or months. Since every person’s experience is unique, getting expert advice is essential to a safer and more comfortable withdrawal process.
Is rapid opioid detoxification harmful to the human body?
Ultra-rapid detox, another name for rapid opioid detoxification, is a contentious and possibly dangerous process. It entails giving naloxone or other opioid receptor antagonists to induce a quick withdrawal while sedated or unconscious. The intention is to expedite the withdrawal process, which should normally be finished in a few hours.
Although the goal of rapid detoxification is to ease people through the uncomfortable withdrawal phase as soon as possible, there are serious risks like cardiovascular risks, respiratory issues, dehydration and electrolyte imbalance, psychological impact, incomplete detoxification, and lack of evidence for efficacy are involved in this process, hence rapid opioid detoxification one of the least recommended method to treat opioid withdrawal.
How does opioid dependence impact individuals?
The effects often permeate many facets of daily life and go beyond the person who is battling with dependence. The following are some effects that opioid dependence may have on individuals:
- Physical Health: Addiction to opioids can cause a decline in one’s physical well-being, raising the risk of overdose, respiratory problems, and infectious diseases like HIV/AIDS.
- Mental Health: People who depend on opioids frequently experience co-occurring mental health conditions like anxiety and depression.
- Financial Strain: Getting opioids illegally or continuing to abuse prescription drugs can be expensive and cause financial strain. People who use drugs may find it difficult to meet their basic needs or may even face legal repercussions.
What is the ideal treatment plan for opioid detox?
A combination of medically supervised detoxification, counseling, medication-assisted treatment (if necessary), education about addiction, holistic methods, family involvement, aftercare planning, and routine monitoring for follow-up care and modifications make up the best treatment plan for opioid detox. For a patient to recover fully, individualized care that takes into account their needs, history, and state of health is essential.
Can a person die from opioid withdrawal?
The symptoms of opioid withdrawal can be extremely painful and upsetting, but the withdrawal itself usually poses no threat to life. Severe complications, however, are possible, particularly if the person has underlying medical conditions or if the withdrawal process is not appropriately managed.
How do families of people dealing with opioid withdrawal get impacted?
Opioid addiction can affect a person’s family as well as themselves profoundly and extensively. The effects often permeate many facets of daily life and go beyond the person who is battling with dependence. Some of the ways family members get affected are:
- Strained Relationships: Opioid dependence can cause emotional distance, communication breakdowns, and conflicts among family members.
- Emotional Toll: As they observe their loved one’s struggles, family members may feel a variety of emotions, such as stress, anxiety, guilt, and frustration.
- Role Reversal: When someone takes on a caregiving role, family dynamics may change, particularly if the person suffering from opioid dependence is unable to carry out their obligations.
Conclusion
The opioid crisis has ensnared individuals and families in its complex web, necessitating our joint attention. The silent battle of opioid withdrawal, a journey filled with physical and emotional pain and a constant reminder of the widespread effects of addiction, is at the center of this fight.
Both legal and illegal opioids provide a momentary reprieve from pain, but they have a cost that goes beyond mere physical well-being. The complex interaction of behavior, environment, and heredity that is opioid addiction knows no bounds and has emerged as a critical public health emergency. As we explore the nuances of opioid withdrawal, a recovery roadmap becomes clear. Important elements of this journey include professional support, therapy, medication-assisted treatment, and acknowledgment.
The timeline for opioid withdrawal occurs in phases, and to guarantee a safer process, expert medical guidance and individualized care are required. Recovering is a team effort that calls for constant assistance, lifestyle modifications, and milestone celebrations. Although setbacks are inevitable, they also present chances for development and resiliency. Withdrawal takes different lengths of time, which highlights the need for individualized care plans and easily accessible treatment options.
Involving yourself in guided treatment programs is the best way to get a structure on what has to be done at what pace.
At Calusa Recovery, we have three opioid treatment programs that are personalized for every individual.
- Outpatient services: Calusa Recovery offers a peaceful setting for a combination of group and individual therapy sessions. Every participant is given a schedule that includes a plan specifically tailored to meet their needs. You can choose between general outpatient care and intensive outpatient treatment during our eight- to sixteen-week outpatient programs.
- Family Therapy: We are aware of how crucial it is for your family to comprehend what you’re going through. Additionally, we support the development of stronger lines of communication between you and your loved ones. You can collaborate to create a happier future when everyone is on the same page. Our mission is to heal you and your loved ones while making sure you have the most robust support system possible.
- Experimental Therapy: We at Calusa Recovery take great satisfaction in being unique in our “out-of-the-box” treatment approaches. Our cutting-edge team includes specialists in NLP (Neuro-Linguistic Programming), recovery coaches, and taking charge of your healing.
You can visit Calusa Recovery Opioid Addiction Treatment for more information and get a personalized plan to cure your opioid addiction.