Are you or a loved one struggling with alcohol addiction? If so, you are not alone. Alcohol withdrawal is a challenging and often overlooked aspect of one’s journey towards sobriety. Understanding how to manage the symptoms and navigate through this difficult phase is crucial for success.
In this article, we will explore the various symptoms associated with alcohol withdrawal and provide practical strategies for managing them effectively. From physical discomforts like tremors and sweating to psychological challenges such as anxiety and depression, we will delve into each aspect and offer helpful tips to alleviate the distress.
Moreover, we will discuss the importance of seeking professional help during the withdrawal process. It is vital to have the support and guidance of experienced medical professionals who can ensure your safety and provide appropriate treatment options.
We understand that embarking on the path to sobriety can be overwhelming, but with the right knowledge and support, it is possible to overcome the hurdles of alcohol withdrawal and achieve lasting sobriety. Join us as we explore this significant topic and equip ourselves with the tools needed for a successful recovery journey.
Let’s start by understanding the key terms and types of drinkers, the differentiation between alcohol abuse, and the often-overlooked topic of alcohol withdrawal.
Defining Alcohol Abuse
Alcohol abuse refers to the excessive consumption of alcohol that leads to negative consequences on an individual’s physical and mental health, as well as their overall well-being. It goes beyond occasional or moderate drinking and becomes a pattern of behavior that can have severe repercussions. Alcohol abuse is often characterized by an inability to control or limit alcohol intake, neglecting responsibilities or relationships due to alcohol, and experiencing withdrawal symptoms when attempting to quit or cut back on drinking.
Alcohol abuse is not limited to any specific demographic or age group, as it can affect people from all walks of life. It is important to recognize the signs of alcohol abuse and understand its effects to take appropriate action and seek help.
The effects of alcohol abuse on the body
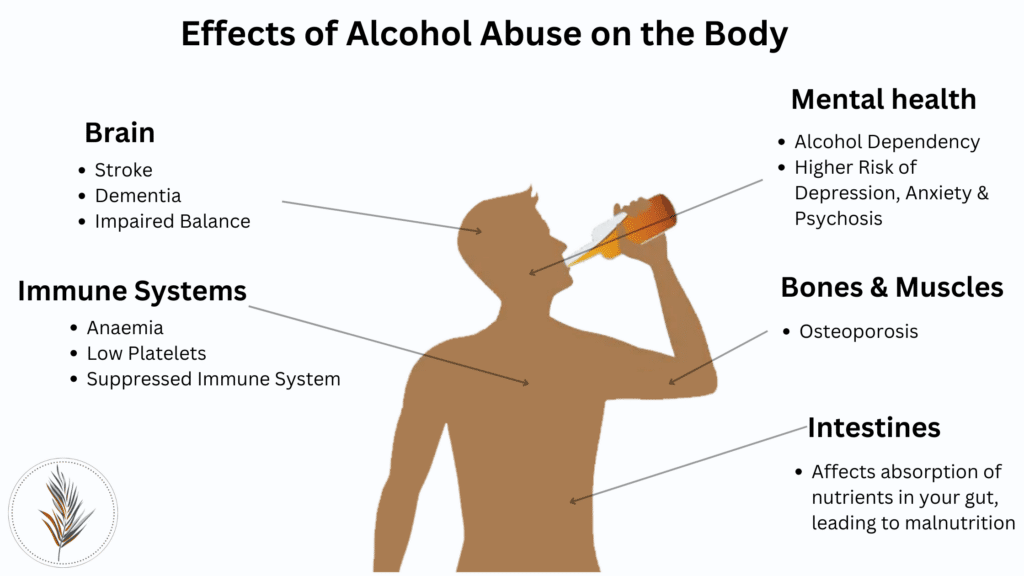
Alcohol abuse can have a significant impact on various organs and systems within the body. One of the most commonly affected organs is the liver. Prolonged alcohol abuse can lead to liver damage, ranging from fatty liver disease to more severe conditions such as alcoholic hepatitis and cirrhosis. These conditions can impair the liver’s ability to function properly, leading to a range of health issues and even liver failure.
Moreover, alcohol abuse can lead to cardiovascular problems. Excessive alcohol consumption can raise blood pressure and increase the risk of heart disease, stroke, and other cardiovascular complications. It can also weaken the immune system, making individuals more susceptible to infections and illnesses.
Additionally, alcohol directly affects brain function. It impairs cognitive abilities, memory, and judgment. Long-term alcohol abuse can lead to structural and functional changes in the brain, resulting in difficulties with learning, concentration, and decision-making. Mental health disorders such as depression and anxiety are also commonly associated with alcohol abuse.
The Psychological Aspects of Alcohol Abuse
Alcohol abuse often stems from underlying psychological factors such as stress, anxiety, depression, or a desire to escape reality. Individuals may turn to alcohol as a coping mechanism, relying on it to numb emotional pain or alleviate feelings of distress. The allure of alcohol lies in its ability to temporarily provide relief and a sense of relaxation.
However, what starts as a temporary escape can quickly develop into a dangerous cycle of dependency. The psychological aspects of alcohol abuse are deeply intertwined with the individual’s emotional well-being. Alcohol becomes a crutch, a means of self-medication that only exacerbates the underlying issues.
Moreover, alcohol abuse can have a profound impact on an individual’s mental health. It can contribute to the development or worsening of mental disorders such as depression and anxiety. The consumption of alcohol alters brain chemistry, leading to imbalances that can further perpetuate psychological distress.
The Physical Aspects of Alcohol Abuse
Long-term alcohol abuse can have devastating effects on the body. Excessive consumption of alcohol can lead to liver damage, cardiovascular problems, and an increased risk of certain types of cancer. The liver, in particular, bears the brunt of alcohol abuse, as it is responsible for processing and detoxifying alcohol.
Chronic alcohol abuse can result in liver diseases such as alcoholic hepatitis, cirrhosis, and fatty liver disease. These conditions can severely impair liver function, leading to a range of health complications and even death. The detrimental effects of alcohol on the liver are well-documented and serve as a stark reminder of the physical toll alcohol abuse takes on the body.
Additionally, alcohol abuse can impair cognitive functioning and lead to memory loss and neurological disorders. Prolonged alcohol abuse can cause brain damage, resulting in difficulties with memory, attention, and problem-solving. These cognitive impairments can have a significant impact on an individual’s ability to function in daily life and can further contribute to the deterioration of personal and professional relationships.
It is important to recognize that alcohol abuse is not solely a personal issue but a public health concern. The psychological and physical aspects of alcohol abuse intertwine, creating a vicious cycle that can be challenging to break. Understanding the complexities of alcohol abuse is the first step toward prevention, intervention, and recovery.
The Causes of Alcohol Abuse
Alcohol abuse can be influenced by a combination of genetic and environmental factors, making it a complex condition to understand. By examining these factors, we can gain insight into the root causes of alcohol abuse.
Alcohol abuse is a multifaceted issue that affects individuals from all walks of life. It is important to understand the underlying causes in order to develop effective prevention and treatment strategies.
Genetic Factors in Alcohol Abuse
Research suggests that genetics play a significant role in an individual’s vulnerability to alcohol abuse. Certain genetic variations can make individuals more susceptible to developing alcohol dependency, while others may offer protection against alcohol-related problems. The interplay between genetics and alcohol abuse is a fascinating area of study that continues to be explored.
Scientists have identified specific genes that are associated with an increased risk of alcohol abuse. These genes influence how the body metabolizes alcohol and how the brain responds to its effects. Understanding the genetic factors involved can help inform prevention and treatment strategies, as well as contribute to the development of personalized interventions.
Furthermore, researchers are investigating the complex interaction between genetics and environmental factors in alcohol abuse. It is believed that certain genetic variations may amplify the impact of environmental factors, making individuals more susceptible to developing alcohol-related problems.
Environmental Factors in Alcohol Abuse
The environment in which individuals grow up and live can greatly influence their relationship with alcohol. Various environmental factors can contribute to the development of alcohol abuse, and recognizing and addressing these factors is crucial in preventing and treating alcohol abuse.
Peer pressure is a significant environmental factor that can influence alcohol abuse. During adolescence, individuals may feel pressured to conform to social norms and engage in risky behaviors, including excessive drinking. The desire to fit in and be accepted by peers can lead to the initiation and continuation of alcohol abuse.
Availability of alcohol is another environmental factor that plays a role in alcohol abuse. Easy access to alcohol increases the likelihood of its misuse, especially among vulnerable populations such as underage individuals. Policies and interventions aimed at reducing the availability of alcohol can help mitigate the risk of alcohol abuse.
Exposure to stressful or traumatic events is yet another environmental factor that can contribute to alcohol abuse. Individuals may turn to alcohol as a coping mechanism to deal with the emotional pain and distress caused by such events. Understanding the impact of trauma and providing appropriate support and resources can help prevent the development of alcohol abuse in these individuals.
It is important to note that environmental factors can interact with genetic predispositions, further increasing the risk of alcohol abuse. For example, individuals with a genetic vulnerability to alcohol dependency may be more susceptible to the influence of peer pressure or the negative impact of stressful events.
In conclusion, alcohol abuse is a complex issue influenced by a combination of genetic and environmental factors. Understanding these causes is crucial in developing effective prevention and treatment strategies. By addressing both the genetic and environmental aspects of alcohol abuse, we can work towards creating a healthier and safer society.
Long-term health consequences of alcohol abuse
The long-term health consequences of alcohol abuse can be devastating. Chronic alcohol abuse significantly increases the risk of developing various types of cancer, including liver, mouth, throat, esophageal, and breast cancer. The carcinogenic properties of alcohol, combined with its impact on the immune system, contribute to the development and progression of these cancers.
Furthermore, alcohol abuse can lead to gastrointestinal problems such as gastritis, ulcers, and pancreatitis. These conditions can cause severe pain, digestive issues, and even life-threatening complications. Alcohol abuse also weakens bones, leading to an increased risk of osteoporosis and fractures.
The effects of alcohol abuse are not limited to physical health. It can have a profound impact on an individual’s mental well-being as well. Alcohol abuse is strongly associated with an increased risk of developing mental health disorders, including depression, anxiety, and alcohol use disorder. These conditions can further exacerbate the negative consequences of alcohol abuse, creating a vicious cycle that is challenging to break.
Understanding alcohol withdrawal
Alcohol withdrawal occurs when a person who is dependent on alcohol suddenly stops or significantly reduces their alcohol intake. This abrupt change disrupts the body’s normal functioning and can lead to a range of physical and psychological symptoms. The severity of these symptoms can vary depending on the individual’s level of dependence and overall health.
During alcohol withdrawal, the body undergoes a period of adjustment as it tries to regain balance without the presence of alcohol. This process can be challenging, and it is crucial to approach it with caution and support. Understanding the symptoms and potential risks associated with alcohol withdrawal is the first step toward managing them effectively.
Alcohol withdrawal symptoms and the dangers of detoxing without medical supervision
For individuals with alcohol dependency, attempting to quit or cut back on drinking can result in withdrawal symptoms. Alcohol withdrawal can be intense and dangerous, requiring medical intervention and supervision. The severity of withdrawal symptoms can vary depending on the level of alcohol dependence and individual factors.
Common alcohol withdrawal symptoms include tremors, sweating, nausea, insomnia, anxiety, and irritability. In severe cases, individuals may experience hallucinations, seizures, and delirium tremens (DTs). DTs can be life-threatening and require immediate medical attention.
Detoxing from alcohol without medical supervision can be dangerous and potentially fatal. It is essential to undergo withdrawal management in a controlled environment, such as a detoxification center or a hospital, where medical professionals can monitor and provide necessary interventions to ensure safety and minimize complications.
What Is Alcohol Withdrawal?
Alcohol withdrawal is a group of symptoms that occur when someone who is both physically and mentally dependent on alcohol stops drinking or cuts back on how much they drink. This experience is known as alcohol withdrawal.

It’s symptoms can range from mild to severe and may include:
- Anxiety
- Sweating
- Tremors
- Nausea
- Vomiting
- Diarrhea
- Headache
- Fatigue
- Insomnia
- Nightmares
- Hallucinations
- Seizures
The severity of alcohol withdrawal depends on some factors, including the amount of alcohol consumed, the length of time the person has been drinking, and their overall health. Alcohol withdrawal can be life-threatening, so it is important to seek medical attention if you or someone you know is experiencing these symptoms.
Alcohol withdrawal symptoms typically begin within 6-12 hours of the last drink and peak within 24-72 hours. However, symptoms can last for several weeks or even months.
Understanding Alcohol Withdrawal
When individuals who have developed an alcohol dependence abruptly stop drinking, they may experience a range of withdrawal symptoms. Understanding the process and symptoms of alcohol withdrawal is crucial for providing appropriate care and support.
The Process of Alcohol Withdrawal
Alcohol withdrawal occurs when the body becomes accustomed to the presence of alcohol and then suddenly has it removed. This can lead to a variety of physical and psychological symptoms as the body adjusts to functioning without alcohol. The severity and duration of withdrawal symptoms can vary depending on the individual’s level of alcohol dependence and overall health.
Symptoms of Alcohol Withdrawal
Withdrawal symptoms can include tremors, sweating, nausea, anxiety, insomnia, and hallucinations. In severe cases, seizures or delirium tremens (DTs) may occur, requiring immediate medical attention. It is important to recognize and address these symptoms promptly to ensure the safety and well-being of individuals going through alcohol withdrawal.
How long does alcohol withdrawal last?
The duration of alcohol withdrawal can vary depending on several factors, including the individual’s overall health, the severity of their alcohol dependence, and the presence of any underlying medical conditions. Generally, the acute phase of withdrawal lasts for about one to two weeks. However, some individuals may experience lingering symptoms for several months.
It is important to remember that the timeline for alcohol withdrawal is not set in stone. Each person’s experience may be different, and it is essential to focus on progress rather than comparing oneself to others. Seeking professional guidance can help individuals navigate through the different stages of withdrawal and provide appropriate support throughout the recovery journey.
How is alcohol withdrawal diagnosed?
Alcohol withdrawal is generally diagnosed in a medical or rehab center — places people go to detox or because their withdrawal symptoms have become a medical emergency. The diagnosis is based on a combination of clinical evaluation, medical history, and an understanding of the individual’s alcohol consumption patterns.
Here are the crucial steps involved in diagnosing alcohol withdrawal:
- Medical History: The healthcare provider will begin by taking a detailed medical history, concentrating on the individual’s alcohol use, including the volume and duration of drinking, as well as any former occurrences of withdrawal.
- Physical Examination: A physical examination is conducted to assess the individual’s overall health and to check for any signs or symptoms of alcohol withdrawal, similar to tremors, increased heart rate, or elevated blood pressure.
- Assessment of Symptoms: The healthcare provider will interrogate the presence and severity of withdrawal symptoms, including anxiety, tremors, sweating, nausea, puking, and seizures. The Clinical Institute Withdrawal Assessment for Alcohol (CIWA-Ar) scale may be used to assess the severity of withdrawal symptoms.
- Blood Tests: Blood tests are frequently performed to evaluate various parameters, including liver function, electrolyte levels, and complete blood counts. These tests can help identify any complications associated with alcohol withdrawal, such as liver disease or electrolyte imbalances.
- Psychosocial Assessment: A psychosocial assessment may be conducted to understand the individual’s mental health, social support, and any co-occurring mental health disorders.
- Assessment for Co-Occurring Conditions: Alcohol withdrawal is generally associated with co-occurring conditions, such as anxiety or depression. These conditions may be assessed to determine the need for more treatment.
- Differential Opinion: The healthcare provider will consider other medical conditions that may mimic alcohol withdrawal symptoms, similar to infections, seizures, or other substance withdrawal syndromes.
- Imaging and Neurological Evaluation: In some cases, neuroimaging or other neurological evaluations may be recommended, particularly if the individual has a history of seizures or other neurological issues.
- Risk Assessment: The healthcare provider will assess the risk of severe alcohol withdrawal, including the potential for delirium tremens (DTs). Factors that increase the risk of severe withdrawal include a history of severe withdrawal episodes, heavy and prolonged alcohol use, and co-occurring medical conditions.
- Treatment Planning: Based on the assessment, the healthcare provider will determine the applicable level of care and treatment. This may include outpatient treatment, inpatient detoxification, and management of withdrawal symptoms with medications.
Alcohol withdrawal timeline
When, for how long, and how severely you feel withdrawal symptoms will depend on your specific situation. Most people recover from their symptoms within a week. And, although your symptoms may not follow this timeline, many people experience withdrawal in three stages.
Below is an abbreviated timeline of these three stages, followed by more information about each one:
- First stage: begins within 6 hours, and can last up to 7 days
- Second stage: starts within the first 48 hours, and can also last up to a week
- Third stage: starts in 48 hours, lasts 2 to 3 days
How to prevent alcohol withdrawal?
The best way to prevent alcohol withdrawal is to avoid drinking alcohol altogether. However, if you have been drinking heavily for some time, it is important to taper off your drinking gradually. This will help to reduce the severity of withdrawal symptoms.
Here are the 6 daily habits that you can practice to be sober and quit alcohol:
- S- Stay Sober- Don’t drink
- O- ounces of water- Drink half your body weight of water
- B- Books- Read at least 10 pages of books daily
- E- Exercise- Workout for at least 15-30 minutes
- R- Reflect- Before going to sleep, write at least 5 things you are grateful for every day.
If you are planning to stop drinking alcohol, it is important to talk to your doctor. They can help you develop a safe and effective plan for tapering off your drinking and managing withdrawal symptoms. The thing of treatment is to help you achieve and maintain soberness, enhance your overall well-being, and reclaim control over your life. It’s important to consult with a healthcare professional to determine the most befitting treatment ground plan for each specific situation.
Managing alcohol withdrawal symptoms at home
While professional medical supervision is recommended during alcohol withdrawal, there are several strategies that individuals can employ to manage their symptoms at home. These strategies can help alleviate discomfort and promote a smoother recovery process. Here are some tips to consider:
- Stay hydrated: Drinking plenty of water can help flush out toxins from the body and minimize the risk of dehydration, a common issue during withdrawal.
- Eat a balanced diet: Consuming nutritious meals can support the body’s healing process and provide essential vitamins and minerals. Include fruits, vegetables, lean proteins, and whole grains in your diet.
- Practice relaxation techniques: Engaging in relaxation techniques such as deep breathing exercises, meditation, or yoga can help reduce anxiety and promote a sense of calm.
- Exercise regularly: Physical activity releases endorphins, which can improve mood and reduce cravings. Engage in activities that you enjoy, such as walking, jogging, or dancing.
- Get enough rest: Rest and sleep are crucial for the body’s recovery. Establish a regular sleep routine and create a comfortable sleep environment to promote better sleep quality.
Remember, these strategies are meant to complement professional medical care and should not replace it. It is essential to consult with a healthcare professional for personalized guidance and treatment options.
There are four types of drinkers – which one are you?
There are four main types of drinkers:
- Social drinkers: Social drinkers drink alcohol in moderation and typically only in social settings. They do not experience cravings for alcohol and can easily go without drinking for long periods.
- Conformity drinkers: Conformity drinkers drink alcohol because they feel pressured to do so by their peers or social group. They may not enjoy drinking alcohol, but they do it to fit in.
- Enhancement drinkers: Enhancement drinkers drink alcohol to enhance their mood or experience. They may enjoy the feeling of intoxication and may drink more than they intended to.
- Coping drinkers: Coping drinkers drink alcohol to cope with stress, anxiety, or other negative emotions. They may use alcohol to avoid dealing with their problems or to numb their pain.
It is important to note that not all drinkers fit neatly into one of these categories. Some people may exhibit characteristics of multiple types of drinkers. Additionally, people’s drinking habits can change over time.
Here are some questions to help you determine which type of drinker you are:
- Do you drink alcohol to socialize or to fit in?
- Do you drink alcohol to enhance your mood or experience?
- Do you drink alcohol to cope with stress, anxiety, or other negative emotions?
- Do you ever find yourself drinking more alcohol than you intended?
- Do you ever experience cravings for alcohol?
- Can you easily go without drinking alcohol for long periods?
If you answered yes to any of the last three questions, you may be at risk for developing alcohol abuse or dependence.
Also, please keep in mind, if you are trying to drink your problems away, it’s not worth it as those problems will still be there in the morning.
What is alcohol abuse?
Alcohol abuse involves immoderate drinking, which is defined as consuming eight or more drinks per week for women and 15 or more drinks per week for men.
Binge drinking, another form of alcohol abuse, is defined as four or more drinks in one sitting for women or five or more drinks in one sitting for men. A person with an alcohol use complaint( AUD) is likely drinking enough to demonstrate alcohol abuse, but it’s possible to abuse alcohol without meeting the individual criteria for an AUD.
Alcohol abuse can also pose a threat to our internal health, leading to anxiety, depression, and indeed dependence.
Here are some red flags of alcohol abuse
- Drinking more or longer than intended
- Having difficulty controlling drinking
- Feeling perverse or anxious when not drinking
- Neglecting liabilities or conditioning due to drinking
- Continuing to drink even when it’s causing problems at work, academy, or in connections.
It’s important to note that alcohol abuse can lead to several serious health problems, including liver complaints, heart complaints, cancer, and internal health problems. Alcohol abuse can be difficult to overcome, but it’s possible with the right support.
It’s not uncommon for individuals floundering with alcohol dependence to be in denial or to repel seeking help. In similar cases, family members can indeed play a pivotal part in seeking support and backing for themselves.
5 crucial ways and strategies for treating alcohol abuse problems:
Honor the Problem
The first step is to admit that there’s a problem with alcohol abuse. This may involve admitting it to yourself or feting it in a loved one.
Seek Professional Help
It’s essential to consult a healthcare professional or dependence specialist. They can give an accurate assessment of the inflexibility of the problem and recommend an applicable treatment plan.
Detoxification(Detox)
For individuals with a significant physical dependence on alcohol, a medically supervised detox may be necessary. This phase involves the gradational elimination of alcohol from the body, frequently with the help of specifics to manage pullout symptoms.
Inpatient or Outpatient Treatment
Treatment options include outpatient recuperation programs( domestic) and inpatient programs. Outpatient programs give 24/7 care and are more suitable for severe cases. Inpatient programs are more flexible and allow individuals to continue with day-to-day life.
Therapy and Counseling:
Therapy and counseling are crucial parts of alcohol abuse treatment. They provide valuable tools to help people overcome their challenges. Three important types of therapy that assist in recovery are:
|
Cognitive-behavioral therapy (CBT) |
Motivational Interviewing (MI) |
Mindfulness-Based Therapies |
| CBT helps people identify the thoughts, feelings, and behaviors linked to their alcohol use. It teaches them to recognize what triggers their drinking and how to deal with those triggers. This therapy empowers them to change their thinking and make better choices. | Open questions, affirmation, reflective listening, and summary reflections (OARS) are the interaction techniques and skills that are used in MI counseling. It supports them in setting realistic goals and building motivation for change. |
These therapies, like Mindfulness-Based Stress Reduction (MBSR), teach techniques to manage stress, anxiety, and cravings. They promote self-awareness and emotional control, so people can make healthier choices. |
Group and individual counseling sessions provide a safe place for people to talk about their concerns and get support. These therapies, along with behavioral treatments, create a complete plan to help individuals recover from alcohol abuse and lead healthier lives.
Medications
Some specifics, like Disulfiram, Naltrexone, and Acamprosate, may be specified to help reduce cravings or discourage alcohol consumption. Drugs should be used in confluence with comfort and remedy.
Remember, the treatment approach may vary based on the existent’s unique circumstances, including the inflexibility of the alcohol abuse, any co-occurring conditions, and particular preferences.
Signs of Drug and Alcohol Abuse
Adolescents who abuse drugs and alcohol are more likely to witness several problems, including
- Unforeseen changes in peers, food habits, sleeping habits, bodily looks, college overall performance
- Irresponsible conduct, negative judgment, and standard lack of interest
- Breaking rules or chickening out from the family
- The presence of drugs packing containers, even though they have no illnesses.
- Bad grades in academics.
- Bloodshot eyes, Laughing for no cause, Loss of interest in sports
- Poor hygiene, lowered public appearance, Avoiding eye contact, Frequent starvation
- The smell of smoke on breath or clothes, Secretive behavior, unusual fatigue.
Several factors can contribute to adolescent drug and alcohol abuse, including:
- Peer pressure
- Family history of substance abuse
- Mental health problems
- Traumatic experiences
- Lack of supervision
However, there are several things you can do to help. If you’re concerned that your child may be abusing drugs or alcohol.
- Talk to them about your concerns
- Set clear rules and expectancies
- Watch their actions
- Seek professional help if demanded
Treatment
If a teen is misusing drugs, you can apply the following approach:
- Have a conversation with your child. Casual drug use can become immoderate or turn into an addiction and result in injuries, legal problems, and fitness issues. Explain to your child about its repercussions.
- Set a good example by drinking responsibly and avoiding drugs.
- Watch your child’s activities and whereabouts.
- Be mindful of the signals and symptoms of drug and alcohol abuse.
- If you think your teen is involved in huge drug use, consult a physician, counselor, or other health care issuer for assistance
Medications for alcohol withdrawal
In some cases, medications may be prescribed to help manage the symptoms of alcohol withdrawal. These medications can help alleviate discomfort, reduce cravings, and prevent potential complications. The specific medications used will depend on the individual’s unique needs and the severity of their withdrawal symptoms.
Common medications used during alcohol withdrawal include benzodiazepines, which can help reduce anxiety and promote sleep, and anti-seizure medications to prevent seizures. Other medications may be prescribed to address specific symptoms or underlying mental health conditions.
It is important to note that medication should only be taken under the supervision of a healthcare professional. Self-medication or misuse of medications can lead to adverse effects and hinder the recovery process.
Long-term effects of alcohol abuse
Alcohol Abuse and Withdrawal are caused by long-term alcohol consumption on health is impacted by the amount of ethanol consumed. While light drinking carries health risks, it’s worth noting that small quantities of alcohol can also offer certain health benefits. However, chronic heavy drinking, frequently associated with alcohol use disorder, results in severe health consequences that outweigh any implicit advantages.
Long-term alcohol consumption is capable of damaging nearly every organ and system in the body. These effects can manifest gradually and may become more severe over time.
The best way to mitigate or prevent these effects is to seek help for alcohol abuse or dependence, either through support groups, counseling, or medical treatment. Reducing or abstaining from alcohol and adopting a healthier lifestyle can significantly improve one’s long-term health outlook.
Alcoholism vs Alcohol Abuse
| S.No | Alcoholism | Alcohol Abuse
|
| 1 | Patterns of Use: Alcoholism, often referred to as Alcohol Use Disorder (AUD), is characterized by chronic, compulsive alcohol consumption with an inability to control drinking. | Patterns of Use: Alcohol Abuse and Withdrawal involves recurrent, excessive drinking that results in negative consequences but does not necessarily indicate an uncontrollable urge to drink. |
| 2 | Loss of Control: Individuals with AUD have difficulty limiting the amount they drink and are often unsuccessful in their attempts to cut back or quit. | Control: Individuals who abuse alcohol may still have some control over their drinking habits. They can choose to cut back or quit if they desire. |
| 3 | Severe Consequences: The consequences of alcoholism are typically more severe and pervasive, impacting various aspects of life, including physical health, mental well-being, relationships, and employment. | Consequences: Consequences of alcohol abuse can include problems in personal relationships, work-related issues, legal trouble, and health complications. |
| 4 | Physical Dependence: Physical dependence is a hallmark of alcoholism. When an individual with AUD stops drinking, they experience withdrawal symptoms, such as tremors, sweating, nausea, and intense cravings. | No Physical Dependence: Those who abuse alcohol do not exhibit physical dependence or withdrawal symptoms when they stop drinking. They can have a drink without experiencing intense cravings. |
| 5 | No Physical Dependence: Those who abuse alcohol do not exhibit physical dependence or withdrawal symptoms when they stop drinking. They can have a drink without experiencing intense cravings. | Tolerance: Over time, individuals with alcoholism develop tolerance, requiring increasing amounts of alcohol to achieve the desired effect. |
| 6 | Compulsion to Drink: Alcoholism is characterized by a compulsive need to drink, even in the face of adverse consequences, and the inability to quit drinking without professional help. | Psychological Dependence: While not physically addicted, individuals may still experience a psychological dependence on alcohol, using it to cope with stress, anxiety, or other emotional issues. |
Creating a sober lifestyle after alcohol withdrawal
Successfully navigating through alcohol withdrawal is just the beginning of the recovery journey. Creating a sober lifestyle is essential for maintaining long-term sobriety. Here are some tips to help you transition into a healthier, alcohol-free life:
- Build a strong support system: Surround yourself with supportive and understanding individuals who encourage your sobriety goals.
- Find healthy coping mechanisms: Identify activities that bring you joy and help you healthily manage stress. This could include hobbies, exercise, or engaging in creative outlets.
- Set goals and celebrate milestones: Establish realistic goals for yourself and celebrate your achievements. Acknowledging your progress can provide motivation and reinforce your commitment to sobriety.
- Practice self-care: Prioritize self-care activities that promote physical, emotional, and mental well-being. This can include getting regular exercise, practicing mindfulness, and engaging in activities that bring you joy.
- Avoid triggers and high-risk situations: Identify triggers that may tempt you to drink and develop strategies to avoid or cope with them effectively. This may involve changing your social circle or finding alternative activities to replace drinking-related events.
Creating a sober lifestyle is an ongoing process that requires commitment, perseverance, and self-reflection. Remember, recovery is a personal journey, and each individual’s path may vary. Be patient with yourself, seek support when needed, and celebrate every step forward.
The Final Say
The road to recovery from Alcohol Abuse and Withdrawal is not easy, but it’s a road worth traveling. It’s a path that involves self-discovery, healing, and resilience.
It’s never too late to stop drinking. The process can challenge your mind and body. When done safely, though, cutting alcohol out of your life can help make you a happy and healthier person. You can repair your body and avoid risks linked to drinking.
It’s a journey that frequently necessitates the support of healthcare professionals, support groups, and loved ones. You can contact Calusa Recovery for more details on alcohol-related issues.